Introduction to Endometriosis and Menopause
Endometriosis is a chronic condition where tissue similar to the uterine lining grows outside the uterus, affecting approximately 1 in 10 women of reproductive age in Canada. It can cause severe pelvic pain, painful periods, and infertility. Menopause, defined as 12 consecutive months without a period, typically occurs between ages 45 and 55, with an average age of 51 in Canada Menopause: A Guide for People With Endometriosis. This phase marks a significant drop in estrogen, often leading to symptom improvement, but for some, challenges persist post-menopause.
What Happens to Endometriosis During Menopause?
Menopause reduces estrogen production, which is crucial for endometriosis, as the condition is estrogen-dependent. For many, symptoms like pelvic pain and heavy bleeding lessen or disappear, but studies estimate that 2-5% of postmenopausal women continue to experience symptoms or develop new ones Endometriosis in Menopause—Renewed Attention on a Controversial Disease. Factors contributing to persistent symptoms include:
- Residual Tissue and Scarring:Endometrial-like tissue and adhesions may remain, causing pain even with low estrogen.
- Hormone Replacement Therapy (HRT): About 30% of women use HRT for menopausal symptoms, and it can reactivate endometriosis, with a recurrence risk up to 4% on unopposed estrogen therapy Endometriosis and HRT.
- Local Estrogen Production: Adrenal glands and fat tissue can produce small amounts of estrogen, potentially sustaining endometriosis.
- Surgical History: Women with severe endometriosis or ovarian surgeries may face earlier menopause or persistent symptoms.
Endometriosis and Early Menopause: The Numbers
Research, including the Nurses’ Health Study II involving over 106,000 women, found a “statistically significant association” between endometriosis and early natural menopause (before age 45) New Research Links Endometriosis with Early Menopause. Specific findings include:
- Women with endometriosis were more likely to experience menopause before 45, especially if never using oral contraceptives or nulliparous.
- For those with ovarian endometriomas, menopause occurred at 42.1 years on average with both ovaries affected, versus 47.1 years with one What Is Perimenopause & How Has It Been Linked To Endometriosis?.
This is significant for Canadian women, as approximately 11% may have endometriosis, potentially affecting reproductive planning.
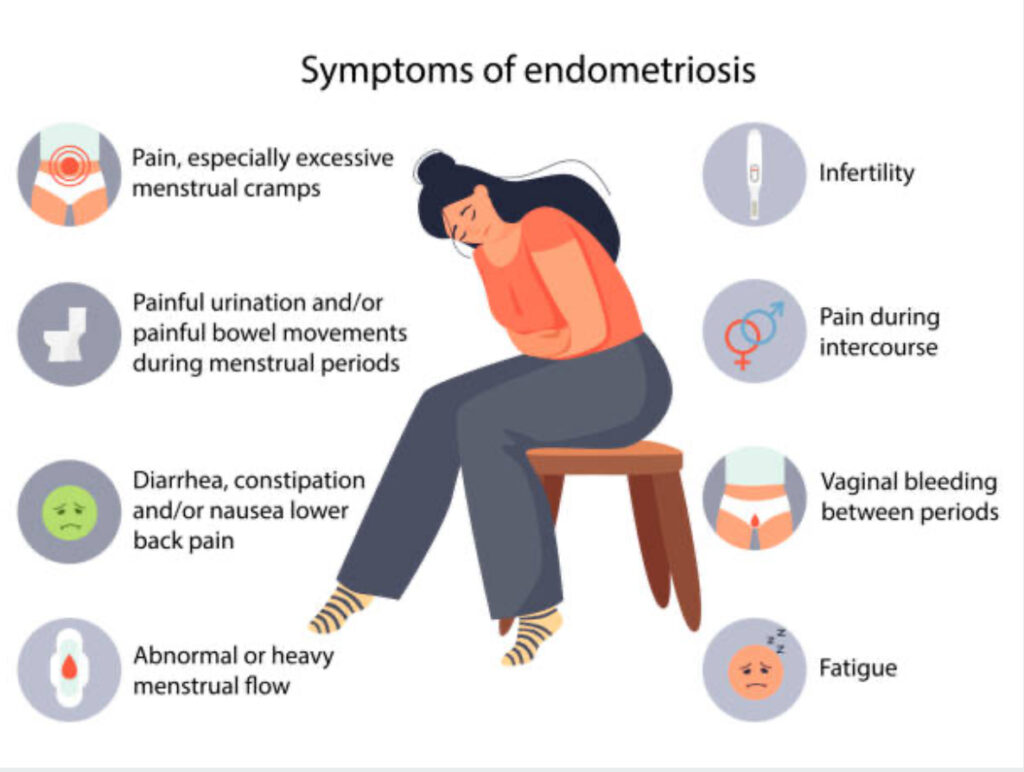
Symptoms of Endometriosis After Menopause
For the 2-5% of women with postmenopausal endometriosis, symptoms can persist or evolve, including:
- Pelvic Pain: A dull ache or sharp discomfort in the lower abdomen or back.
- Bowel or Bladder Issues: Pain during urination or bowel movements, especially if affecting the gastrointestinal tract or urinary system.
- Fatigue: A lingering effect of chronic inflammation.
- Painful Intercourse: Less common but possible if deep lesions remain.
A 2019 systematic review found that in 61% of 36 documented cases, symptoms started over 10 years after menopause, suggesting delayed onset possibly due to genetic or epigenetic changes Symptomatic endometriosis developing several years after menopause in the absence of increased circulating estrogen concentrations: a systematic review.
Risks and Complications
Postmenopausal endometriosis carries several risks:
- Malignant Transformation:Endometriosis increases the lifetime risk of ovarian cancer by 1.96 times, with about a 1% progression rate to cancer, particularly clear cell and endometrioid types Endometriosis After Menopause: Risks, Treatment, Complications & More. Case reports note instances in women on HRT.
- Recurrence: In a review of 42 cases, recurrence occurred in some on estrogen-only HRT, highlighting a small risk Endometriosis in Menopause—Renewed Attention on a Controversial Disease.
- Cardiovascular and Bone Health: Early menopause from surgeries raises osteoporosis and heart disease risks. Canadian data shows women with endometriosis have a 1.5 times higher heart disease risk and 1.2 times higher stroke risk, with 1 in 12 Canadian adults having diagnosed heart disease Menopause: A Guide for People With Endometriosis.
Diagnosis in Postmenopausal Women
Diagnosing endometriosis after menopause is challenging due to overlapping symptoms. Methods include:
- Pelvic Exam: Checks for masses or tenderness.
- Imaging: Transvaginal ultrasound (TVS) detects 70-90% of ovarian endometriomas, and MRI offers detail for deep infiltrating endometriosis Endometriosis After Menopause: A Rare Diagnosis Worth Considering.
- Laparoscopy: The gold standard, confirming endometriosis in most cases via biopsy, essential for ruling out malignancy.
Treatment Options
Management focuses on symptom relief and risk reduction:
- Surgery: Excision removes implants, reducing pain and cancer risk, while hysterectomy/oophorectomy may be considered for severe cases, triggering immediate menopause if not already present Diagnosis and management of endometriosis.
- Medications: NSAIDs like ibuprofen help manage pain, and low-dose combined HRT or tibolone can control symptoms, with aromatase inhibitors used off-label but potentially causing bone loss.
- Lifestyle Changes: Anti-inflammatory diets, regular exercise, and stress management (e.g., yoga) may reduce symptoms by 20-30%, though evidence is limited.
HRT and Endometriosis: Weighing the Pros and Cons
HRT relieves menopausal symptoms for 80% of users but may reactivate endometriosis in 2-4% with a history. Canadian guidelines suggest:
- Combined HRT: Preferred over estrogen-only, reducing recurrence rates from 9.5% to under 2% in studies Endometriosis and menopause—management strategies based on clinical scenarios.
- Lowest Effective Dose: Minimizes risks while managing symptoms.
- Monitoring: Regular check-ups every 6-12 months for women on HRT.
Discussing with healthcare providers is crucial, balancing benefits like 50% reduced osteoporosis risk against endometriosis risks.
Living Well with Endometriosis Post-Menopause
For the 2-5% affected, consider:
- Stay Informed: Join online communities for real-time support, as only 17 studies globally estimate prevalence Endometriosis in Menopausal Women—A New Age Is Coming? Literature Review.
- Advocate for Yourself: Seek specialists, as only 20% of general gynecologists are trained in advanced excision techniques.
- Track Symptoms: A diary can pinpoint triggers, aiding 60-80% in tailoring treatment.
Self-Care Tips for Managing Endometriosis Post-Menopause
- Stay Active: Regular exercise can help manage weight, improve mood, and reduce pain.
- Healthy Diet: Eat a balanced diet rich in fruits, vegetables, and whole grains to support overall health.
- Stress Management: Practice relaxation techniques like yoga, meditation, or deep breathing to reduce stress.
- Sleep Well: Aim for 7-8 hours of sleep each night to help manage pain and improve energy levels.
- Connect with Others: Join support groups or online communities to share experiences and learn from others.
- Regular Check-ups: Keep up with medical appointments to monitor your condition and adjust treatment as needed.
By taking an active role in your health and working closely with your healthcare team, you can effectively manage endometriosis during and after menopause.
Conclusion
Endometriosis doesn’t always resolve with menopause. While 95-98% of women see improvement, the 2-5% with persistent or new symptoms—potentially affecting millions in Canada—need tailored care. Early menopause risk, heart disease (1.5 times higher), and ovarian cancer risks (1 in 52 vs. 1 in 75) underscore vigilance. With surgery, adjusted HRT, or lifestyle tweaks, relief is possible. You’re not alone—use this knowledge to navigate confidently.
Key Citations
- Endometriosis in Menopause—Renewed Attention on a Controversial Disease
- Symptomatic endometriosis developing several years after menopause in the absence of increased circulating estrogen concentrations: a systematic review
- What Is Perimenopause & How Has It Been Linked To Endometriosis?
- Endometriosis in a postmenopausal woman without previous hormonal therapy: a case report
- Endometriosis After Menopause: Risks, Treatment, Complications & More
- Endometriosis in Menopausal Women—A New Age Is Coming? Literature Review
- Menopause: A Guide for People With Endometriosis
- Endometriosis and HRT
- Endometriosis and menopause—management strategies based on clinical scenarios
- New Research Links Endometriosis with Early Menopause
- Association Between Laparoscopically Confirmed Endometriosis and Risk of Early Natural Menopause
- Endometriosis and Early Menopause
- Practices and Attitudes Concerning Endometriosis Among Nurses Specializing in Gynecology
- The management of menopause in women with a history of endometriosis: a systematic review
- What Is Perimenopause & How Has It Been Linked To Endometriosis?
- Nursing care for patients with endometriosis and/or adenomyosis: A mixed methods systematic review protocol
- Endometriosis in Menopausal Women—A New Age Is Coming? Literature Review
- Diagnosis and management of endometriosis
- Endometriosis: diagnosis and management
- Endometriosis: An update on diagnosis and medical management
- The Menopause Foundation of Canada
- Endometriosis